Callie Blackwell watched helplessly on as her son came so close death that doctors said there was nothing left to do but pray.
It’s understandable, then, that she has become such a huge advocate for the medical intervention that brought him back from the brink.
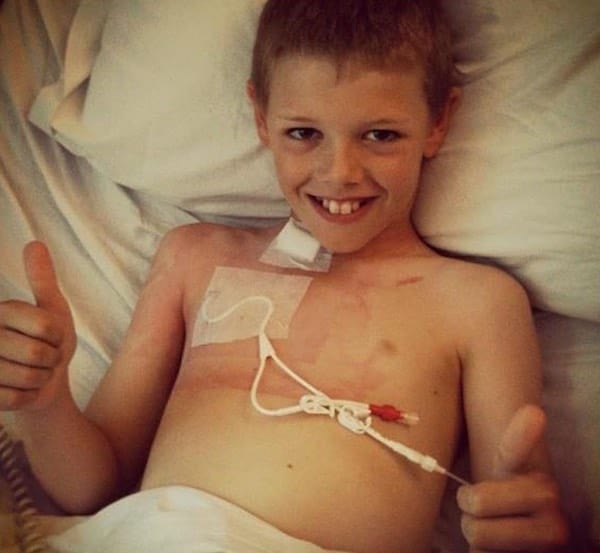
After four failed transplants, young Deryn (pictured above on the right, with his mum and brother) lay gravely ill in hospital, having battled leukaemia and being left with no bone marrow. A cocktail of pharmaceutical drugs had left him in a comatose state.
Some months earlier, Callie used natural products including Manuka honey to help reduce Deryn’s virus count. With every other option seemingly exhausted, she decided to try something she had, until that point, only ever read about online – cannabis.
“I just thought I may as well try it, we had nothing to lose at that point. So I tried cannabis tincture and within half an hour I saw a difference. Shortly afterwards, Deryn was refusing morphine and pharmaceutical drugs.
“Five days later, we saw his bone marrow kick in. I continued to use cannabis three or four times a day with him and he came off all of the other drugs,” she recalls.
“The medical team said it was scientifically impossible, ‘it’s a miracle, there’s no other explanation’. Obviously I couldn’t tell them what I had given him but I knew cannabis had saved his life.
“Since that time, I’ve spoken to his doctors about it and most were quite open to the idea, but one of them just puts his fingers in his ears.
“He just does not want to hear about the very thing that saved my son. To help people have the choice to use cannabis that they are currently being denied is what inspires me every day.”
Callie documented Deryn’s miraculous recovery in her book, The Boy in Seven Billion.
In the six years since his survival, he has regained use of both his knee and hand which medics warned would be lost forever.
His mum, meanwhile, has become a prominent campaigner for the medical use of cannabis and for people to be allowed to produce cannabis themselves.
Indeed, the right to ‘grow your own’ is the focus of Callie’s indomitable efforts on behalf of families across the UK.
 “I want people to be able to grow their own without fear of prosecution. Prohibition causes fear and paranoia comes from the fact growing cannabis is illegal.
“I want people to be able to grow their own without fear of prosecution. Prohibition causes fear and paranoia comes from the fact growing cannabis is illegal.
“I used to grow my own for Deryn in my shed and every time I heard a noise I was worried it was the police and I was going to be arrested.
“But not only would they take my son’s medicine away, they would take my son away and put him into care.”
In fact, so great were Callie’s fears of prosecution over growing cannabis, that they triggered a nervous breakdown.
“Every time I spoke to someone who came to me for support, and who I would help under the radar, I wondered whether they were secretly a police officer.
“That is an awful situation for anyone to be in and I know because I have been there.
“But ultimately, my need to tell people about cannabis and to help people was something I couldn’t keep to myself.
“Now, I believe being so vocal about it is almost a form of protection for me.”
Having long spoken out about growing her own cannabis, Callie now encourages others to follow her lead.
“I actively encourage people who come to me for help to grow their own cannabis as it’s the only way to ensure you have your own supply and that you know what you’re getting.
“It’s very important for safety and for harm reduction. It’s really not advisable to get it from a street dealer as you have no idea where it has come from,” she says.
“From a cost perspective, it’s much cheaper to grow your own – street cannabis can cost anything up to £20 a gram – and you can make your own bespoke strain.
“There are over 5,000 strains and you have to find what works for you. For Deryn, I recently grew him some lemon diesel oil, which he knows is very good for mental health and it works well for him.
“It’s very important that you try different strains and find what works for you, then you can have your own supply.
“However, I do think that it’s such a shame that the situation remains that while I’m very openly growing my own, telling the whole of Charing Cross police station what I’m doing after I was arrested for protesting outside Parliament, nothing happens to me.
“If it did, I’d make sure I went down kicking and screaming and making a real fuss.
“But if the man down the road wants to grow a bit of cannabis, he’d be arrested and made an example of. That’s very frustrating and it’s not fair.”

Callie is keen to help other families benefit from cannabis medicine.
While legalisation of growing your own cannabis is her goal, Callie is adamant it should be done in the best interests of those who will benefit from it on a human and medical level; rather than corporate businesses who will profit financially.
“We know the corporations are going to come in to this debate, but it must not be to the detriment of people who have been researching and living in this area for 50 years of their lives.
“We have become the experts and we know what we are doing better than they do.
“We don’t want it to be legalised with parameters that suit the Government and the pharmaceutical companies.
“We want people’s health to be put back into their own hands so they can be left alone and be healthy.
“There are so many conditions which could be treated by people on their own rather than going to the NHS for help – we would save the NHS a huge amount of money if we were allowed to grow our own.
“But we also have to be careful that if this does become reality that we have the provisions in place to protect us and our rights.
“It cannot be a case of you’re allowed to do it but you can only grow one strain and buy equipment from these certain shops.
“This has to be beneficial to all of us and we have to be allowed to discover what benefits us for ourselves.”
Callie’s motivation is simple, she says – helping people in ways she can.
“I believe in freedom of choice and to be given autonomy over our own bodies. If people want to have a vaccination or they don’t, that’s fine.
“But people have a choice. And I believe that should be the case with cannabis,” she says.
“I was in the healthcare system for five years with Deryn and I know the incredible amount of stress it causes for your child to be so ill, and the stress that is caused by using and growing the medicine you know has saved his life.
“I get 10 or 15 messages on average every day from families who are desperate for help, and as well as helping to supply them with oils, I guide them through the grow your own process.
“I always say, ‘I can’t save you, but I can help you to save yourself’. I try and guide them all the way through so they can be self sustaining.
“When you’re in a medical situation you give over so much power to doctors, but by growing your own and self sustaining, that’s an important part of the healing process. Having this power to do this for yourself is a very important thing.”
 Cannabis Health is THE UK magazine covering cannabis medicine and wellbeing from every angle. It is affiliated with the Medical Cannabis Clinicians Society and lists campaigner Hannah Deacon, leading expert Professor Mike Barnes and prominent doctor Dani Gordon on our editorial panel. For a limited time only, we are offering a free – absolutely no strings – annual subscription to the quarterly print title. You will receive four issues, delivered with discretion to your address – with no hidden fees or obligation to pay beyond that. To repeat, this is a 100% free promotion available to the first 100,000 sign-ups.
Cannabis Health is THE UK magazine covering cannabis medicine and wellbeing from every angle. It is affiliated with the Medical Cannabis Clinicians Society and lists campaigner Hannah Deacon, leading expert Professor Mike Barnes and prominent doctor Dani Gordon on our editorial panel. For a limited time only, we are offering a free – absolutely no strings – annual subscription to the quarterly print title. You will receive four issues, delivered with discretion to your address – with no hidden fees or obligation to pay beyond that. To repeat, this is a 100% free promotion available to the first 100,000 sign-ups.
Claim your free subscription now!

 News6 months ago
News6 months ago
 News6 months ago
News6 months ago
 Science5 months ago
Science5 months ago
 Industry6 months ago
Industry6 months ago
 News6 months ago
News6 months ago
 News5 months ago
News5 months ago
 Health4 months ago
Health4 months ago
 News5 months ago
News5 months ago
 “I want people to be able to grow their own without fear of prosecution. Prohibition causes fear and paranoia comes from the fact growing cannabis is illegal.
“I want people to be able to grow their own without fear of prosecution. Prohibition causes fear and paranoia comes from the fact growing cannabis is illegal.
 Cannabis Health is THE UK magazine covering cannabis medicine and wellbeing from every angle. It
Cannabis Health is THE UK magazine covering cannabis medicine and wellbeing from every angle. It