Case Studies
Two years on: what happened to our prescription bid?
Published
3 years agoon

It’s been two years since medical cannabis was legalised in the UK but all of these children – and dozens more – have been refused a prescription on the NHS. We asked why.
On 1 November 2018 medical cannabis campaigners celebrated. The treatment that was saving the lives of their loved ones was finally legalised in the UK, after months of rallying politicians, national TV appearances and telling their heartbreaking stories to the press. No one thought that two years on they would still be fighting.
In the two years since the legalisation only three NHS prescriptions have been issued and parents have spent tens of thousands of pounds funding their child’s medication each month. Some have sold their homes, begged friends and family for money, risked everything pursuing legal action and spent the hours that they should have been with their sick children calling for change.
Seven families from the End our Pain movement, initially set up to campaign for the law change, told us why they have been refused access on the NHS.
 Bailey
Bailey
It’s November 2018. A then 16-year-old Bailey, is in the high dependency unit at his local hospital having another seizure. His mum, Rachel Rankmore and dad, Craig Williams, have been up for 48 hours straight monitoring their son in case the unimaginable should happen.
A consultant neurologist chooses this moment to ask the family if they want to have a conversation ‘about the other stuff?’
Rachel knows what they mean.
Her son has been taking hemp oil for two years but despite making huge improvements at first, his condition has plateaued. He is now having hundreds of seizures a day. He needs full extract cannabis oil.
Bailey has a rare form of epilepsy known as Lennox Gastaut Syndrome. For most of his life he has had to wear a crash helmet to protect his head from drop seizures, and being blue-lighted to hospital has been a weekly occurrence.
Before he tried Charlotte’s Web CBD, doctors told Rachel and Craig there was nothing left they could do.
“The hospital offered to give us epidiolex [a drug containing CBD which was approved for use in the UK last year], but we knew we needed full extract cannabis oil,” remembers Rachel.
“I asked them why they wouldn’t prescribe when they knew there was nothing left for Bailey to try.
“At first they said it was because THC would ‘damage his brain’, but when I pushed them the answer I got was that they helped write the BPNA (British Paediatric Neurology Association) guidelines and couldn’t go back on them.”
BPNA guidance for clinicians says that products with ‘higher proportions of THC (>0.2%)’ have ‘no randomised controlled clinical trial evidence of safety or efficacy’ in children and young people with epilepsy.
It adds that clinicians should not feel ‘under pressure’ to prescribe cannabis based medicines until they have undergone clinical trials.
Rachel asked for a second opinion from another neurologist at the hospital. Again the answer was no.
Bailey has had a private prescription for medical cannabis for two years now. He has had no emergency trips to the high dependency unit, a reduction in his antiepileptic drugs, he is attending school, engaging, interacting in conversations, voicing what he wants, playing computer games and going out with his support workers. As Rachel says ‘living his best life’ for the first time in 16 years.
His prescription is only afforded through the fundraising efforts of his friends, family and followers, but due to the coronavirus restrictions they haven’t been able to organise any events this year. The funds for Bailey’s medication will run out in December.
Rachel has been told by a hospice that when he inevitably ends up in hospital with uncontrollable seizures the most likely line of treatment would be anesthetic and pain management.
“They would write my son off rather than give him a prescription for a medicine that has proved to work for Bailey, that is perfectly legal and he has obtained privately for over a year,” she says.
“Our son’s life is in danger because the law passed and guidance written have failed him.
Murray
Karen Gray was also told by her consultant that he wouldn’t prescribe full-extract cannabis for her son Murray, eight, due to the BNPA guidelines.
Murray, who has Doose Syndrome has been seizure-free for 17 months since he started taking full extract cannabis oil.
He looks unrecognisable to how he did before. He is speaking, attending school and no longer needs the use of a wheelchair.
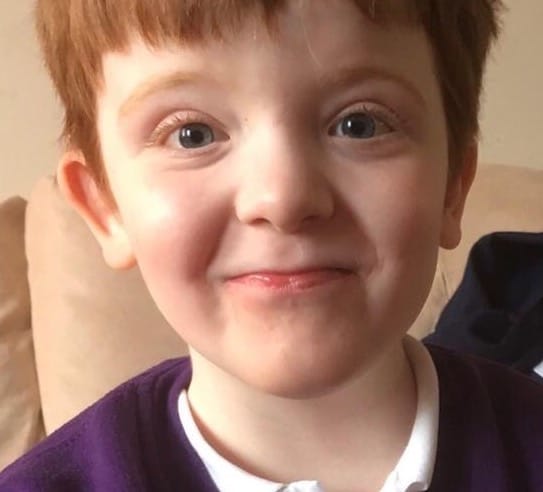 But when his case was referred to the Refractory Epilepsy Specialist Clinical Advisory Service (RESCAS) it was recommended that he be weaned off the oils and put back on epidiolex.
But when his case was referred to the Refractory Epilepsy Specialist Clinical Advisory Service (RESCAS) it was recommended that he be weaned off the oils and put back on epidiolex.
Karen says she has always accepted the consultant’s decision not to prescribe, but refuses to take him off his current medication, when epidiolex had previously left him in epileptic status and confined to a hospital bed.
“He’s always said he doesn’t want to go against his peers, which I’ve always accepted, but I obviously wasn’t going to change anything when Murray has been seizure-free since June 2019,” she says.
“I asked for the RESCAS decision to be appealed so I could pursue a shared care agreement [which enables access to a prescription through the NHS].”
Murray’s consultant recently resigned from his care claiming the ‘stress of the situation’ was putting him under too much ‘strain’.
He is now under the care of the ‘complex epilepsy team’ made up of several neurologists, who have said they feel it would be ‘reasonable’ to put Murray’s case to RESCAS again in six to 12 months.
“That’s another six to 12 months of us funding his prescription ourselves,” says Karen, who currently struggles to find the £1,400 a month.
“We can’t afford this long-term but we’re terrified that if we take him off it he will start having seizures again.”
 Ben
Ben
A lack of clinical trials is one explanation for the NHS not prescribing, which comes up often.
Joanne Griffiths is also trying to pursue a shared care agreement for her son Ben, 11, but is fighting a losing battle. She first asked for full-extract cannabis following the law change in 2018 but says she got ‘a flat no’.
“I was told they had a clear policy that they were not going to prescribe these drugs until more trials were done.
“They constantly quoted the BPNA guidance,” says Joanne.
She and her husband considered going down a judicial route but decided it would be better to work with the doctors, who had cared for Ben, who has severe epilepsy, cerebral palsy and autism, all his life.
“We were eventually discharged with a letter saying we had asked for THC products that were ‘illegal to prescribe’ – which they weren’t,” she continues.
“Every child is different but Ben wasn’t being treated as an individual.”
A year down the line Joanne has just received a letter from the Greater Preston Clinical Commissioning Group (CCG) declining her funding request for a shared care agreement between Ben’s GP and private neurologist, as it was ‘contrary’ to policy and no grounds for ‘clinical exceptionality’ were found.
Joanne is now considering legal action.
“It’s the only thing I can do,” she says.
“They know that Ben has got no other treatment line left.”

Charlie
One family who are taking this very risk is Matt and Ali Hughes, parents to three-year-old Charlie.
Before they discovered cannabis medicine last May, Charlie, who was diagnosed with West syndrome at 10 weeks old, was having up to 120 seizures a day. Now they are down to between 10 to 20.
The couple are seeking a judicial review of the NICE (National Institute for Health and Care Excellent) guidelines which prevent doctors in the NHS prescribing medical cannabis and leave them forced to fund the £1,200 prescription each month.
NICE has acknowledged the need for more research into the use of medical cannabis and supports NHS England’s call to collect evidence from randomised controlled trials and observational studies.
But the guidelines state that until there is clear evidence of the safety and effectiveness of cannabis-based medicinal products, specialist doctors need to consider individual patient circumstances and risks and benefits in choosing treatments.
Matt and Ali will argue that the existing evidence – while mostly anecdotal and low quality – should be enough to support doctors to prescribe full extract cannabis oil for severe treatment-resistant epilepsy.
If they are successful the guidance could be redrafted, which they hope would give some doctors the confidence to write the prescription.
“I’ve spoken to clinicians that say they would prescribe if they could but I think there is a feeling that if they step out of line, their trust will block it anyway,” Matt told Cannabis Health earlier this year.
“A lot of clinicians are prescribing it privately, just not on the NHS. So why is it fine for children to take it privately but for the NHS we need all this extra evidence?”
 Zak
Zak
In 23-year-old Zak’s case, it wasn’t so much that his doctor didn’t accept that there was evidence out there, but that they ‘didn’t have time’ to read it.
“I’ve asked our consultant several times why they won’t prescribe on the NHS,” says Zak’s dad, Benedict Lamb.
“They always say that the research hasn’t been done to prove that it’s safe.”
Benedict continues: “As parents we’ve become quite knowledgeable about the subject. Over the last 15 years in Canada and Israel there have been several published studies. I told them all the research exists, but they said they didn’t have time to read it.”
Benedict feels lucky in a way, even though Zak has Dravet Syndrome and autism and is severely disabled, he has responded well to epidiolex where many children do not.
Age 15, doctors told the family he only had six to 12 months to live, but thanks to the medication eight years on he is very much alive, attending a specialist college and continuing to make improvements.
CBD saved Zak’s life, but he still has seizures. And with every seizure there is a risk that he might not come back from it.
“Every time they have a seizure, it comes with the risk of more damage to the brain, nervous system or even death,” says Benedict.
“When he was younger Zak used to have very serious fits on a regular basis, but thankfully that’s stopped since he was put on epidiolex.
“Although he still has seizures, they are all around the three minute mark, which means that he doesn’t end up in hospital. We’re in a much better place than we were, but he hasn’t got any better.
He adds: “The goal for all of the parents in the group and beyond is for our children to be seizure-free.”
It is hoped that an oil with a higher concentration of THC will help to control Zak’s seizures and he is now due to trial a new product, which has been funded by the pharmaceutical company for six months.
But then what?
“They could turn around and say its X amount,” says Benedict.
“And then we’re faced with balancing the financial stress against our child’s health.”
 Fallon
Fallon
“It’s all about the money,” according to Fallon’s mum, Elaine Levy.
If anyone should know it’s her.
Elaine sold her house to fund her daughter’s medical cannabis prescription with the financial pressure of finding the £2,200 each month leaving her “broken” – both emotionally and financially.
The family are now staying at Elaine’s sister’s flat, with no idea how long it will be until they can look to find a place of their own.
Fallon, 27, who has had Lennox–Gastaut syndrome since the age of four, went from being ‘zombie-like’ on a cocktail of antiepileptic drugs and barely able to leave the house, to enjoying a full day out with her family for the first time thanks to medical cannabis.
Elaine says Fallon’s former consultant, who is one of the country’s leading epilepsy specialists, has tried ‘every way he can’ to help them.
“When we got the letter from NHS England to say we could have medicinal cannabis, Bedrolite was on the tarif as one of the drugs we could have,” she says.
“He wrote the request out there and then and within half an hour he received a response refusing it.
“Then he put in an independent funding request to show that Fallon is different and exceptional, but this was also declined by the CCG.”
Elaine has tried Fallon on a cheaper oil but it wasn’t as effective and she couldn’t bear to watch her daughter falling over and ‘smashing her face on the floor’ several times a day.
She now just has a few weeks of Fallon’s medication left and doesn’t know what will happen after that.
It was suggested that if she films Fallon falling over when she is off the oil, this may help build her case.
But Elaine believes that the ‘excuses’ about a lack of evidence, are just masking the real problem – that it’s too expensive to fund on the NHS.
“There is so much evidence, we are the evidence,” she says.
“It’s not about the guidelines, it’s about the money and everything else is just muddying the water.
“The NHS has not got the budget for it. Too many people would need it and they would be inundated.”
A leading pharmacist is said to have told Elaine that she ‘shuddered’ when Sajid Javid legalised medical cannabis, knowing that there wouldn’t be the funding.
It came as no surprise to Elaine.
She adds: “My consultant said to me in his own words when I left his office for the last time, if it was ‘£5 a bottle I would be prescribing it for everyone who needs it with intractable epilepsy’ – which says it all really.”

Eddie
Back in 2018 Ilmarie Braun still had hope. She was alongside other parents, including Hannah Deacon, who were tirelessly campaigning for the law change.
“For a while it all moved fast and things felt really positive, it felt like we were being listened to,” she says.
Ilmarie and her husband Alex met with MP Nick Hurd, who at the time was setting up a panel of specialist epilepsy experts to deal with cases ‘just like Eddie’.
Eddie, five, was given a diagnosis of West syndrome at seven months old. He spent the first years of his life on up to five different types of antiepileptic drugs until his parents tried him on Hayley’s Hope CBD from America.
As he was weaned off the pharmaceuticals, with no deterioration in his condition, they saw his personality emerge for the first time.
But the CBD alone wasn’t enough to control his seizures.
Eddie’s pediatrician agreed to put an application in to RESCAS, but refused on the grounds that it wasn’t written by a neurologist and Eddie hadn’t yet tried epidiolex (despite the fact it hadn’t yet been approved for use in the UK).
When he started to plateau on the epidiolex, they asked again for a prescription of full extract cannabis oil. Their consultant took their request to the drugs and therapeutics committee at their local hospital. A panel of eight said no, unanimously.
According to Ilmaire, the pharmacist felt it would have been ‘immoral’ to ask them to write Eddie a prescription when they had already obtained a private prescription from a neurologist in London.
“They all claim to have every sympathy with us – we get all these different people saying we really feel for your family and what you’re going through – but they really don’t,” she says.
Ilmarie accepts the fact that theirs was a small hospital and staff didn’t feel they could be the first to prescribe when specialist centres such as Great Ormond Street were refusing.
She finds it harder to accept that the Government could do something to alleviate some of these families’ suffering, but chooses not to.
“There’s a huge amount of politics involved. Matt Hancock promised that he would help us and he hasn’t,” she says.
“Our doctors won’t even tell us whether our kids are going to be teenagers – we don’t know how long we have and yet they’re telling us we need to worry about possible psychosis later on down the line – it makes no sense.
“We don’t know what the future holds, but we know it’s not going to be easy. We’re angry that the Government won’t do something to alleviate that.”
Ilmarie speaks for many when she says a breakthrough feels as far away as it ever did.
“There’s a real mismatch between what was promised and what the reality is,” she adds.
“This is not what anyone was campaigning for.”
What the Department of Health told us:
The Department of Health is said to be ‘working closely’ with NHS England-NHS Improvement (NHSE-I) and the National Institute of Health Research (NIHR) to establish the clinical trials needed to ‘develop the evidence base to support further commissioning decisions’.
It adds that NHS funding decisions follow ‘clearly developed procedures’ that ensure the fair distribution of funding – prioritising medicines that have proved their safety, quality and efficacy. The latest NICE guidelines demonstrate a ‘clear need’ for more evidence to support prescribing and funding decisions, as the majority of THC/CBD products are unlicensed and have not demonstrated clear evidence of their ‘safety, clinical and cost effectiveness’.
RESCAS was established to support clinicians to ‘optimise treatment’ of refractory epilepsy but the service is ‘advisory only’ and the responsibility remains with the patient’s neurologist.
“We sympathise with patients dealing with challenging conditions and the decision on whether to prescribe medicinal cannabis is ultimately one for clinicians to make,” said a Department of Health and Social Care spokesperson.
“Since the law changed, two cannabis-based medicines have been made available for prescribing on the NHS for patients with multiple sclerosis or hard to treat epilepsies, where clinically appropriate. This follows clear evidence of their safety, clinical and cost effectiveness.
“However, more evidence is needed to routinely prescribe and fund other treatments on the NHS and we continue to back further research and look at how to minimise the costs of these medicines.”
Sarah Sinclair is a respected cannabis journalist writing on subjects related to science, medicine, research, health and wellness. She is managing editor of Cannabis Health, the UK’s leading title covering medical cannabis and CBD, and sister titles, Cannabis Wealth and Psychedelic Health. Sarah has an NCTJ journalism qualification and an MA in Journalism from the University of Sunderland. Sarah has over six years experience working on newspapers, magazines and digital-first titles, the last two of which have been in the cannabis sector. She has also completed training through the Medical Cannabis Clinicians Society securing a certificate in Medical Cannabis Explained. She is a member of PLEA’s (Patient-Led Engagement for Access) advisory board, has hosted several webinars on cannabis and women's health and has moderated at industry events such as Cannabis Europa. Sarah Sinclair is the editor of Cannabis Health. Got a story? Email sarah@handwmedia.co.uk / Follow us on Twitter: @CannabisHNews / Instagram: @cannabishealthmag
You may like
-


Greek Health Minister to Speak in London About Greece’s Groundbreaking Medical Cannabis Programme
-


Dr Franjo Grotenhermen: “Cannabis gave me a new reason to live”
-


Recreational cannabis use may protect against cognitive decline – study
-


Call for funds to kickstart UK medical cannabis awareness campaign
-


Study examines risk of CUDs among medical cannabis patients
-


UK cannabis clinic expands to offer mental health treatments
Recent Articles
- Greek Health Minister to Speak in London About Greece’s Groundbreaking Medical Cannabis Programme
- Dr Franjo Grotenhermen: “Cannabis gave me a new reason to live”
- Recreational cannabis use may protect against cognitive decline – study
- Call for funds to kickstart UK medical cannabis awareness campaign
- Study examines risk of CUDs among medical cannabis patients
- UK cannabis clinic expands to offer mental health treatments
Trending
-

 Industry6 months ago
Industry6 months agoFirst UK-grown cannabis medicine expected by end of 2023
-

 News6 months ago
News6 months agoUK government accepts ACMD recommendations for CBD products
-

 News5 months ago
News5 months agoEurope’s first legal cannabis dispensaries to open under sixth Swiss pilot
-

 News6 months ago
News6 months agoUK government to permit electronic prescribing of cannabis medicines
-

 Science4 months ago
Science4 months agoMedical cannabis doesn’t impair cognitive function – study
-

 Industry5 months ago
Industry5 months agoFirst Jersey-grown medicinal cannabis product to hit UK market
-

 News5 months ago
News5 months agoFive years of medical cannabis, five NHS prescriptions – how did we get here?
-

 Patients6 months ago
Patients6 months ago“They just didn’t care” – cannabis patient arrested on driving lesson speaks out
