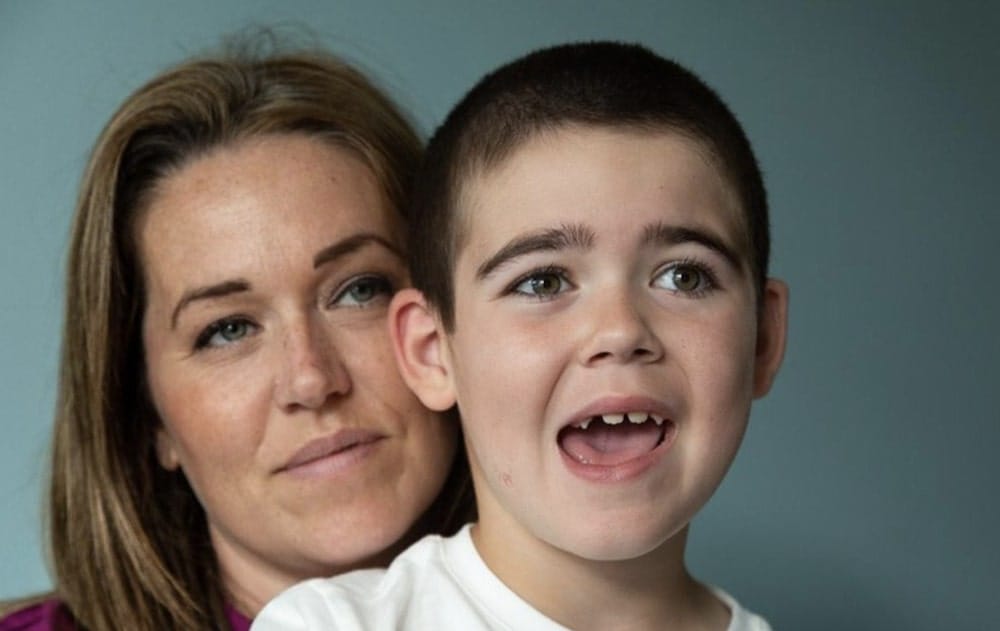
Mother and prominent campaigner, Hannah Deacon has pleaded with the Prime Minister to help secure access to medical cannabis for her son and other patients.
Hannah Deacon has been left fearing for her nine-year-old son, Alfie Dingley’s life after his life-saving cannabis medication was stopped because of Brexit.
Supplies of certain cannabis oils, which are imported from the Netherlands, have been terminated following the end of the Brexit transition period on 31 December, leaving dozens of families without access to life-saving medication.
Over 40 patients who have been prescribed certain cannabis-based medicines (CBMPs) in the UK but can only obtain their prescription through the Transvaal pharmacy, which is based in the Netherlands.
Hannah and other patients in the same position, were given just two weeks notice by the Department of Health and Social Care (DHSC) – and were only made aware of the change through a letter sent to UK importers, clinics and patient groups, which she has described as “disgraceful”.
It stated that prescriptions issued in the UK ‘can no longer be lawfully dispensed in an EU Member State’ meaning dispensing Bedrocan products in the Netherlands for UK prescriptions is ‘no longer an option’ from 1 January 2021.
Alfie Dingley, nine, who has a rare form of severe epilepsy, became the first UK child to receive a permanent license for medical cannabis, following Hannah’s high profile campaign to help change the law in 2018.
He is now prescribed Bedrolite oil on the NHS – the medication recommended by his doctor – but Hannah says she only has around six weeks of supplies left.
Before beginning treatment with the oil Alfie’s life had been dominated by clusters of epileptic seizures that began at just eight months old. On one occasion this resulted in a three-week stint on life support in intensive care.
He has now been almost completely seizure free for well over a year and is able to attend school and live a relatively normal life.
But Hannah fears that stopping his treatment could be catastrophic.
“Without access to his medication Alfie would likely go back to having dozens of seizures, any of which could potentially be life-threatening,” she said.
“The progress he has made on Bedrolite is amazing, why would they take away a medicine that is working?”
The DHSC has advised pharmacies to find “alternative” prescriptions to switch patients onto, but as Hannah points out, each variety of cannabis medicine is different and what works for one patient does not necessarily work for another.
“A clinical decision to prescribe Bedrolite has been made by Alfie’s doctor and to change it to anything else would be dangerous,” she continued.
“Just because an oil has CBD and THC in it doesn’t mean it’ll have the same effect.”
Professor Mike Barnes, founder of the Medical Cannabis Clinicians Society, who obtained the first full license to prescribe medical cannabis in the UK, explained: “Each variety of cannabis is subtly different and you can’t just swap a child from one product to another.
“It shows an astonishing level of ignorance to think that every cannabis product is the same when there are 147 different cannabinoids in each plant.”
Prof Barnes described the situation as “appalling”.
He added: “It is not an exaggeration to say that one or two children will die if they can no longer access this medication.”
Hannah has contacted Boris Johnson directly and is now making a public plea to him and Health Secretary Matt Hancock to step in and find a permanent solution.
“I am very fortunate to have an NHS prescription for Alfie, but now it feels as though we are back at square one, after years of fighting for access to this life-saving medication for us and other families.
“The COVID pandemic has shown that the Government is willing to take any action necessary to protect lives. This is not about politics, children are at risk.
“I will fight this all the way and I urge Boris Johnson to step in, work with the Dutch Government and help us.”
In a statement released on Wednesday 6 January, the Centre for Medical Cannabis (CMC) said it was “concerned” by reports that UK patient’s supplies to medical cannabis have been cut off.
The CMC says it has engaged with the DHSC throughout 2020 to find alternative products that may be “suitable for substitution under careful medical supervision”, for patients who will be affected.
It continued that the situation illustrates the need for a “broad and customised range of cannabis medicines” that can be “rapidly and cost effectively” imported into, or developed and produced within the UK.
“Supply issues and discontinuations of medicines have always been a difficult challenge for the medical community to deal with, especially when dealing with vulnerable patients who are stabilised on a particular medicine,” explained Dr Andy Yates, pharmacy lead for CMC.
“This situation is exacerbated when you are dealing with a complex medicine such as CBMPs. Working with our members, we have been able to provide the DHSC with a list of CBMPs that may be suitable for substitution, but as the article points out they do have differences in composition and would therefore require careful medical management if a solution to supplying Transvaal products cannot be found.”
The centre has advised families to seek alternative legal routes to obtaining cannabis based medicines in the UK, although this is currently only possible through private prescriptions.
In a response to Cannabis Health, a DHSC spokesperson said: “We sympathise with patients dealing with challenging conditions and there is a range of alternative cannabis-based medicines available to UK patients.
“The decision on what treatments to prescribe to patients is rightly one for clinicians to make, on a case-by-case basis and dependent on the specific needs of the individual.
“If patients have any concerns, they should discuss them with their doctor.”

 News6 months ago
News6 months ago
 News6 months ago
News6 months ago
 Science5 months ago
Science5 months ago
 Industry6 months ago
Industry6 months ago
 News6 months ago
News6 months ago
 News5 months ago
News5 months ago
 Health4 months ago
Health4 months ago
 News5 months ago
News5 months ago