Rebecca Allen-Tapp reveals the role cannabis has played in helping her heal, after being diagnosed with a rare cancer at the age of 30.
“I’ll try and give you the summarised version,” says Rebecca Allen-Tapp, whose life changed forever, when doctors found a golf ball size tumour in her lung in 2018.
Her health had become progressively worse following the birth of her son the year before, but her story starts much earlier, in her teenage years.
Rebecca, who was living in her home state of Washington in the US at the time, had been plagued by depressive episodes and anxiety since she hit puberty. The symptoms would be so extreme that she would be forced to take time off school and later – when they continued into her 20s – weeks at a time off work.
Doctors ran tests but never found anything wrong, so “chalked it up to hormones”. Even a therapist struggled to identify the cause of her sadness, diagnosing her with bipolar disorder, despite the fact she showed no signs of the manic highs associated with the condition.

“Doctors were dismissive, because they couldn’t figure out what was wrong,” she says. “As a woman I was not listened to, it was just downplayed, which led to a lot of distress afterwards.”
During her pregnancy though, Rebecca felt the best she had in years.
“I felt comfortable and well-rounded for the first time in my life,” she says. “I’m probably one of the few women who enjoyed being pregnant.”
But just a week after her son was born, things began to deteriorate. She started experiencing ocular migraines where she would lose her vision, her blood pressure went through the roof, and the suicidal thoughts returned.
“I started doing my own research and took all this information to my doctor,” she explains.
“I said ‘I think I have what’s called PMDD [premenstrual dysphoric disorder]. They agreed to assess me and I actually had 10 of the 11 classic symptoms of PMDD.”
This diagnosis brought Rebecca some clarity, but in the background she was still struggling with her physical health. In July 2018, she developed pneumonia which she couldn’t seem to shake.
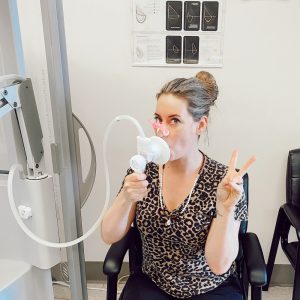
Rebecca had struggled with her health for several years before her diagnosis
“The pneumonia never went away,” she continues. “I started having X-Rays and they could see signs of it in the lung but they said it just needed time to repair…fast forward to October and it was hurting to breathe during a normal day of work or yoga, it wasn’t normal.”
Despite this, she put off having a CAT scan, planning to go back in the New Year after the busy Christmas period. She was only 30 after all, she didn’t think it was urgent.
But Rebecca’s symptoms worsened and two weeks after Christmas she found herself calling an ambulance, unable to move her arm.
“My lung lining was so inflamed that it was actually hurting my shoulder, it’s called pleurisy and it’s actually quite a common phenomenon,” she says.
That’s when they found the tumour.
She adds: “My doctor wasn’t incredibly worried at first, because cancer just wasn’t on their radar and I thought ‘it doesn’t just happen like that, right?’”
A rare and “misunderstood” cancer
Neuroendocrine cancer is an extremely rare and – in Rebecca’s words – “misunderstood” cancer, caused by tumours growing in the neuroendocrine cells, which have similar traits to those of nerve cells and hormone-producing cells. Only around 20 per cent of neuroendocrine cancer patients have a tumour in the lung.
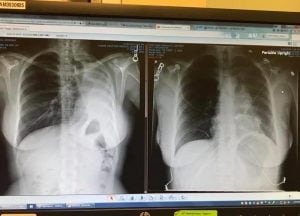
She ended up having her left lung amputated
Luckily, Rebecca’s tumour had a very low malignancy, but doctors believe it had been growing for 10-15 years before it was discovered.
Neuroendocrine tumours tend not to respond to traditional treatments such as radiation and chemotherapy, so the best route was surgery. In February 2019, despite her surgeon’s best efforts, they ended up taking out her whole left lung.
“I’ll never forget the moment where I woke up and turned to my husband and said ‘how much did they take? And just the look on his face when he had to say they took the whole thing,” she says.
“I tried not to let it get to me, and I still don’t today, because it was the best course of action.”
Rebecca made progress quickly and remarkably was home the next day, where cannabis became a big part of her recovery.
“I leaned on cannabis heavily during my recovery,” she says.
“I used tinctures to help with the pain but I thought I’d probably have to couple the cannabis with other painkillers, but I didn’t. That’s really where I started to really understand the way cannabis could be used as a medicine.”
Discovering cannabis as a medicine
As well as her physical recovery, cannabis has played – and continues to play – a big part in maintaining Rebecca’s mental equilibrium too.
Survivors of neuroendocrine cancer have to live with the knowledge that it can return at any time, to any part of the body.
“For the rest of my life, the reality is that I have to get scanned and it could be anywhere at any time, I might not even know that it’s present,” she explains.
“There’s Rebecca before the diagnosis, and Rebecca after the diagnosis, it’s almost like everything goes into slow motion, you start to realise that time is fleeting and that crazy things can happen to you.
“You start to battle that paranoia, because you fear that you are going to get struck by lightning twice.”

She adds: “At the time that they found it, I didn’t have any metastasis, so I didn’t have any other tumour locations, and usually by that point, it would have had some other activity somewhere else. But is that to say that there’s not one somewhere else that I don’t know about?”
Cannabis has helped Rebecca find a sense of normalcy again, reducing her anxiety levels and helping her focus on what’s important so she can take care of herself properly.
“They’ve tried to prescribe heart medication, muscle relaxers, painkillers and anti-anxiety medicines, but I don’t want them. I use one plant for it all and it does the trick. It’s so versatile, I don’t know where I would be without it,” she says.
Her physical symptoms, which include tachycardia, raynaud’s, shortness of breath, severe heartburn and fatigue are all compounded by stress, so maintaining a good work-life balance and keeping her anxiety levels down is vital.
“Stress is one of the biggest drivers, we’re all desensitised to stress but the impact is real,” says Rebecca.
“If I’m not making time for myself and I’m putting too much into my day and constantly chewing on things mentally, I see that taking its toll on my body.”
She continues: “My mind is like a browser with 15 tabs open. I feel like cannabis is what closes those tabs down. It helps me prioritise what’s most important. I always joke that I feel like I have the ‘Good Wolf’ and the ‘Bad Wolf’ in my brain and never know which one to feed. Cannabis helps me feed the Good Wolf.”

The root cause?
At first glance, it might seem like Rebecca’s tumour and the PMDD that has afflicted her for much of her life are unrelated. But a self-confessed “science nerd” she has been studying herself for long enough to have reason to believe her symptoms are connected by a root cause; hormone dysregulation.
“My body responds negatively to hormone dysregulation and it’s something that I’m still battling to this day, there are times that I can’t get out of bed for days on end,” she says.
“I started tracking my cycle and recording notes on anything that bothers me and I started to notice patterns about when it was happening based on the time of the month.
“I don’t know the correlation and it’s really hard to pinpoint, but I definitely notice what time of the month it is.”
She adds: “I think the tumour was more of a byproduct of the larger root cause, which is hormone dysregulation and inflammation. I think this created the opportunity to develop a tumour microenvironment.
“I’m in a lot of neuroendocrine support groups and so many of those with tumours in their lungs are women.”
Eat, sleep and breathe cannabis
Rebecca has made a career out of cannabis, first the states working in sales and marketing, before moving into the post-extraction side and co-owning a processing lab. Having recently moved to the UK with her family, she’s keen to bring her expertise to this side of the pond – as both a patient and a professional.

Rebecca forged a career in the cannabis sector, first in the US and now here in the UK
She is working as business development manager for Asahi Glassplant UK and recently joined the PLEA (Patient-Led Engagement for Access) advisory board.
“I eat, sleep and breathe cannabis,” she says.
“It’s a very different market, but I feel what spans the borders is the stigma facing patients. There are people who could really benefit from using cannabis that aren’t using it and need someone to champion that way for them.”
She adds: “It might not be the answer for them, but for others it will be life-changing.”
Home » Health » “I don’t know where I’d be without cannabis,” says cancer survivor

 News6 months ago
News6 months ago
 Science5 months ago
Science5 months ago
 Industry6 months ago
Industry6 months ago
 News6 months ago
News6 months ago
 News5 months ago
News5 months ago
 Health4 months ago
Health4 months ago
 News5 months ago
News5 months ago
 Health3 months ago
Health3 months ago


















