A UK medical cannabis company says it can provide products for patients whose supply has been cut off by Brexit, but experts caution that they may not be ‘like-for-like replacements’.
Medical cannabis distributor, Grow Pharma has announced it has trialled the UK’s first extraction of a cannabis based medicine in a licensed facility, since GW Pharmaceuticals.
The company is taking efforts to replicate cannabis-based medicinal products to patients whose supply from the Netherlands has been disrupted due to Brexit.
Over 40 patients who have been prescribed Bedrocan oils in the UK, but can only obtain their prescription through the Transvaal pharmacy in the Netherlands, were left without access to the treatment after the end of the Brexit transition period on 1 January 2021.
Last week the Dutch government confirmed it will continue to supply the medication for UK prescriptions until 1 July 2021, while a long-term solution is reached.
Now Grow Pharma, which says it is already legally importing GMP produced Bedrocan flowers into the UK for distribution to patients, claims it can offer these families an “alternative option”.
Its partner pharmacy, IPS Pharma, says it will produce the cannabis oils in its EU GMP certified production facility in Surrey, at a lower price point than what patients were paying for the equivalent medicine from The Netherlands.
“Although it has been announced that a temporary solution has been found and companies are working on a longer term solution which may take months, a post Brexit, sustainable and UK based solution for this problem is needed and we are ready to step up to help,” said CEO of Grow Pharma, Pierre van Weperen.
He also claimed that when prescriptions come in, initial samples will be made available free of charge and the cost moving forward will be “significantly less” than parents are used to paying.
“We are ready to help these children and their parents and offer them an alternative option,” added van Weperen.
“This is an opportunity to establish a UK-based solution that can produce CBMPs to the highest possible standards.”
But clinicians and experts in paediatric epilepsy have warned that ‘significant risk’ remains in switching medications for children with refractory epilepsy, even to a similar product, as each strain of cannabis is subtly different.
In a statement, Ashok Patel, pharmacist at IPS Pharma said there was “no reason” that products would “differ significantly” aside from “fluctuations” in the production process.
“We will be using the exact same starting material these patients are used to,” he commented.
“From a scientific standpoint there is no reason why the end result would differ significantly beyond any fluctuations that may have arisen already within the current production process.”

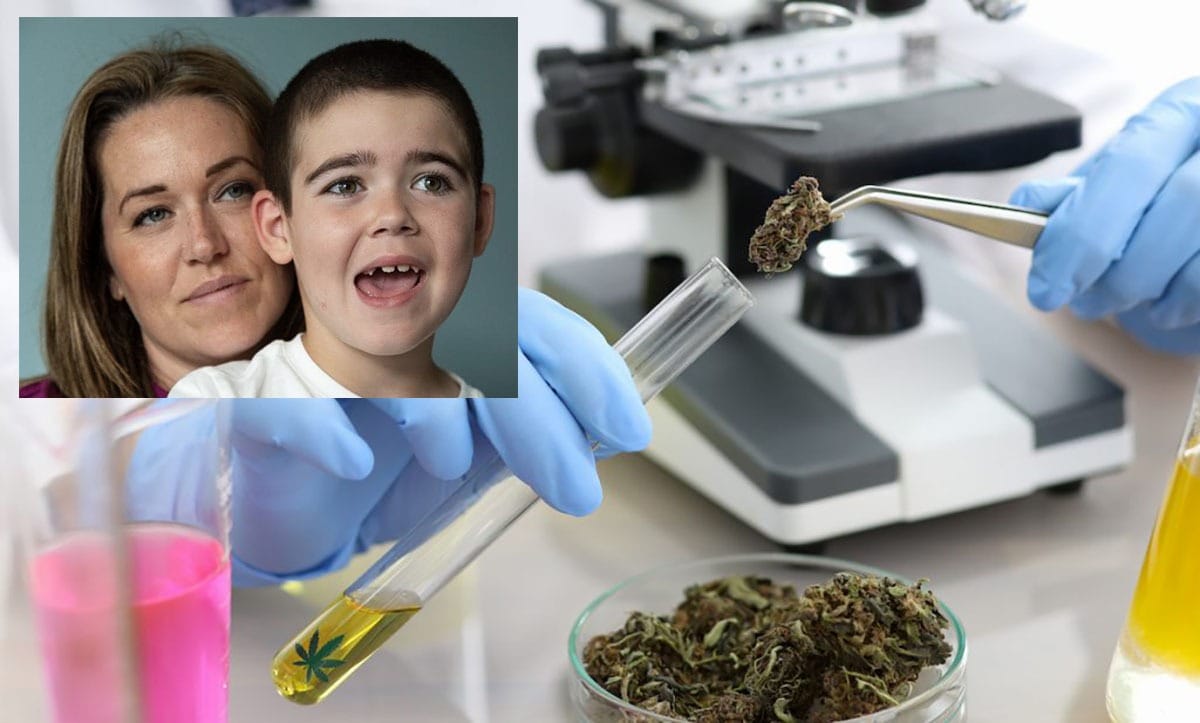
Hannah Deacon and son Alfie Dingley.
Hannah Deacon, who has campaigned for access to medical cannabis for her son Alfie, welcomed the fact that these companies were stepping up to help, but stressed that these products may not be a ‘like-for-like replacement’.
“It is great that these companies are coming forward and offering to help, but in its statement IPS admits that there will be fluctuations in the production process and that does not give me faith that these medicines will protect my child from suffering a worsening of seizures,” she said.
Earlier this month paediatrician and epilepsy specialist at The Neurology Centre of Toronto, Dr Evan Lewis warned of the risks of switching medications in children with severe epilepsy.
“It is imperative that children who are benefiting from a particular medical cannabis product are not changed to another product,” he wrote in a statement to UK leaders.
“It can be highly unsafe and could result in worsening seizures, or breakthrough seizures.”
Lewis went on to say that if breakthrough seizures occur and a child is switched back onto their previous medication, it does not always work and the seizures may become more difficult to control.
Deacon, a co-founder and director of cannabis consultancy firm Maple Tree continued: “If you ask any clinician, they will strongly advise that you do not change medication for any reason if a child is stable.
“The best outcome would be for Bedrocan products from the Netherlands, or a like-for-like product, to be produced here in the UK.”
Professor Mike Barnes, co-founder of the Medical Cannabis Clinicians Society added that it is not only the ratio of THC to CBD which is important, but all of the cannabinoids and other terpenes which make up the product.
“All of the cannabinoids and terpenes in the cannabis plant have medical value, which is why it’s so important that we understand fully what is in the product,” he said.
“Each variant of cannabis is different – you even get differences between batches – so a product can have the same ratio of THC to CBD, but to ensure these products were safe for children we would need to see a certificate of analysis to show that they have tested all of the terpenes and other compounds as well.”

 News6 months ago
News6 months ago
 Science5 months ago
Science5 months ago
 Industry6 months ago
Industry6 months ago
 News6 months ago
News6 months ago
 News5 months ago
News5 months ago
 Health4 months ago
Health4 months ago
 News5 months ago
News5 months ago
 Health3 months ago
Health3 months ago