A survey of more than 1,000 practicing UK GPs, suggests that 73 percent would be open-minded about prescribing medical cannabis.
Results from the UK’s largest ever survey on attitudes towards medical cannabis among GP’s, indicate that almost three quarters were open-minded about having a more active role within the field.
When asked if they would support the idea of trained, specialist GPs facilitating prescriptions for eligible patients, 39 percent of respondents answered with yes, while 34 percent said they weren’t sure and only 26 percent said no.
In addition, almost a quarter (24 percent) of respondents said they would be willing to take on the role of prescribing and overseeing medical cannabis treatments.
The survey, published on Monday 12 July, by The Primary Care Cannabis Network (PCCN) is the first insight into UK GP’s attitudes towards medical cannabis.
Over half believe cannabis-based medicines could benefit patients who have exhausted conventional treatments, while 27 percent feel it can offer improved quality of life.
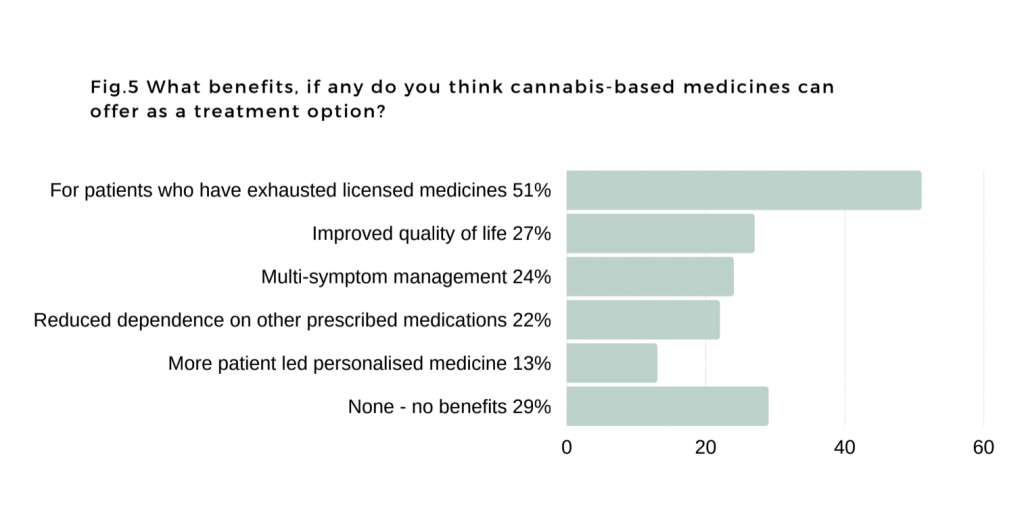
Credit: PCCN
Just under a quarter believe it can offer multi-symptom management and reduced dependency on other prescribed medications, while 13 percent believe it can offer more patient-led personalised medicine.
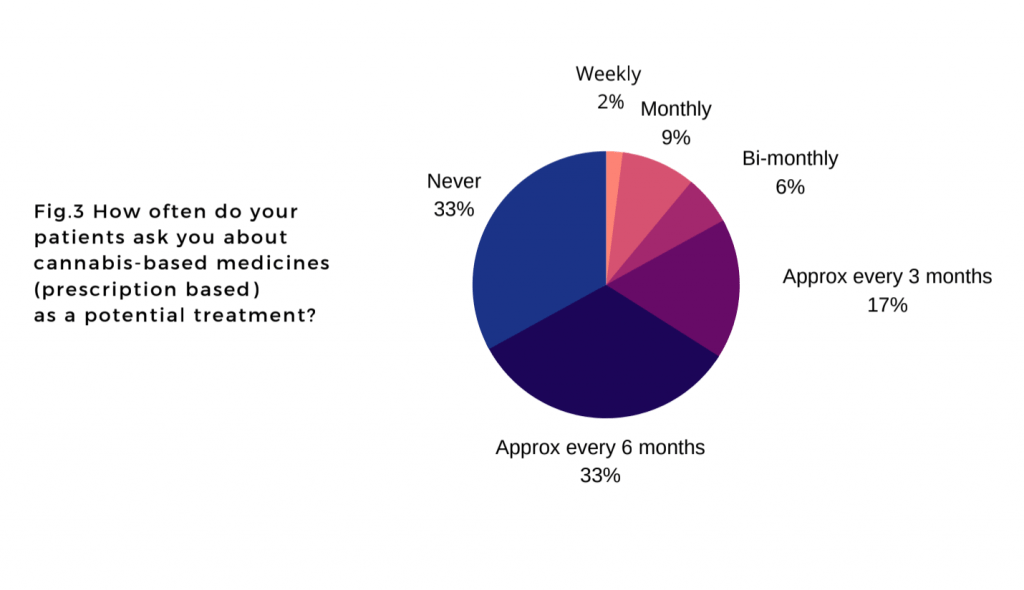
A third of GPs (33 percent) said they were asked about medical cannabis treatment by their patients approximately every six months, but access for UK patients remains extremely limited, with most prescriptions of unlicensed cannabis medicines having been issued by specialist consultants working within private clinics.
With at least 1.4 million people in the UK thought to be self-medicating with cannabis, GPs could have a significant role to play in initiating access and overseeing prescribing for a wide range of conditions that are commonly managed within a primary care setting, such as chronic pain and anxiety, say the authors.
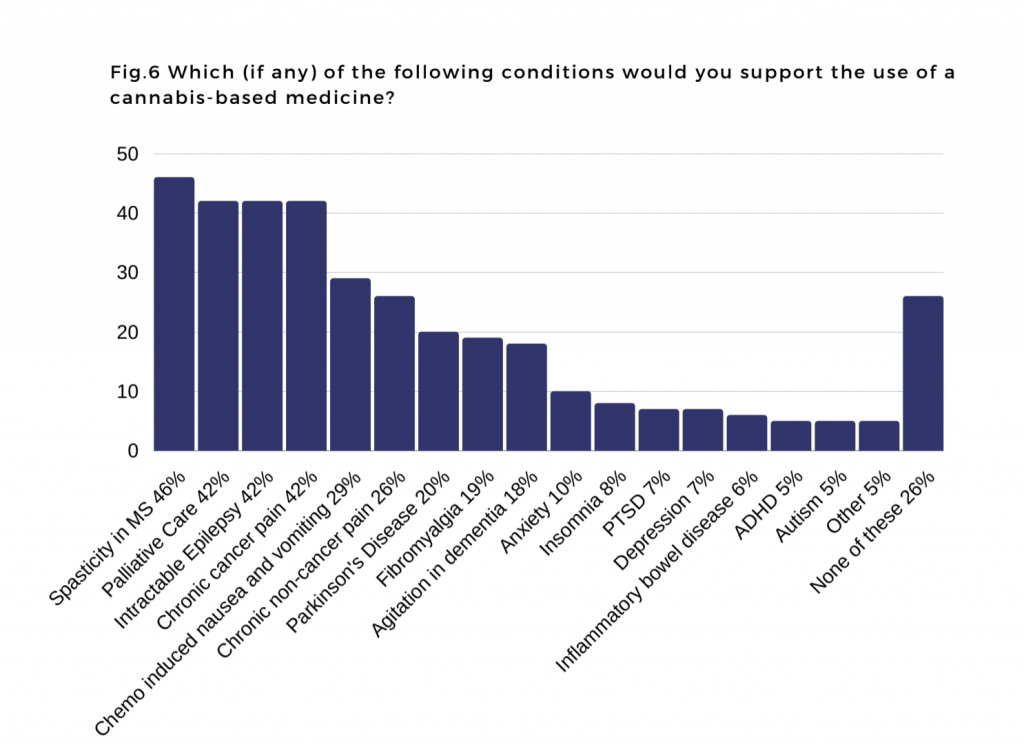
Credit: PCCN
According to the survey, UK doctors favoured medical cannabis for use in chronic cancer pain, palliative care, intractable epilepsy, and spasticity in multiple sclerosis (MS), all of which – apart from epilepsy – can be managed within primary care.
However, mood disorders such as anxiety, depression, and PTSD were not generally seen as suitable indications for medical cannabis treatments, despite growing numbers of patients being prescribed privately for these conditions.
The majority of doctors (72 percent) cited their main concern around cannabis-based treatments as the fact that the majority of the available medicines are unlicensed.
Lack of evidence around efficacy also continues to be a problem.
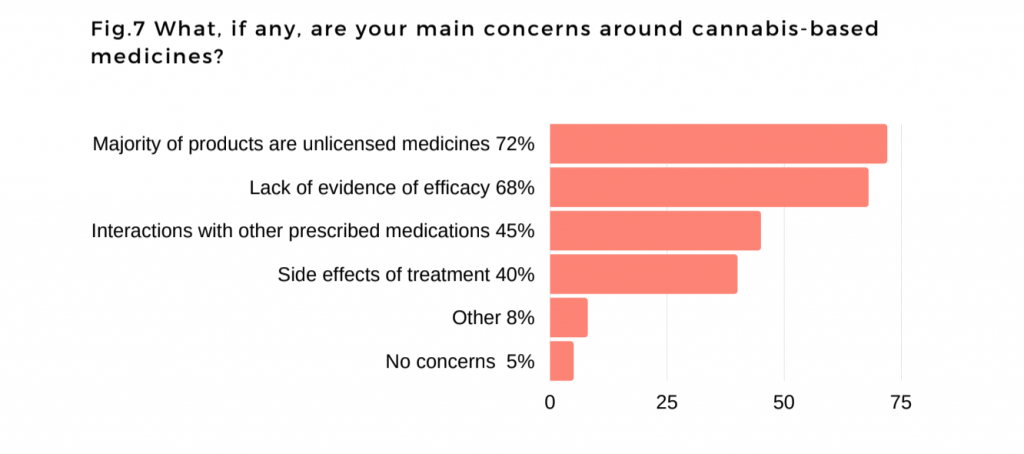
Credit: PCCN
Those behind the survey say more awareness and access to education for GPs is crucial, with 48 percent of respondents asking for clear and concise summaries of the most up to date evidence-based research on cannabis-based medicines.
GP focused e-learning platforms and quick reference desktop guidance were also called for.
Founder of the PCCN, the UK’s largest network of GPs with a professional interest in learning about medical cannabis, Dr Leon Barron explained: “GPs make up the majority of medical cannabis main prescribers in many of the more established legalised medical markets.

Dr Leon Barron, founder of the PCCN
“They can enable patient access to this medicine in Canada, USA, Germany and Australia to name a few countries. In the UK however, GPs have largely been left out of the conversion and we feel it’s time to change that.”
While the survey points to some positive attitudes among doctors in the UK, it highlights the need for standardisation in how GPs approach the subject of cannabis medicines with their patients.
As they are often the first port of call, GPs can offer a patient a positive – or negative – experience when enquiring about medical cannabis.
Patient advocacy group PLEA (Patient-Led Engagement for Access) has called for doctors to educate themselves to be able to provide a more open environment to discuss cannabis medicines.
PLEA advocacy lead, Lucy Stafford says she was lucky that her GP was open-minded and helped her find a specialist prescriber.
“GP knowledge is crucial. Having a GP that is non-judgmental, supportive, and open to understanding medical cannabis could lead to the patient discovering a treatment that works for them as I did,” she commented.
“I was lucky to have an open-minded GP who referred me to a specialist prescriber – the difference in how I am able to live now after treatment is like night and day.
Credit: PCCN
“Doctors always ask for evidence but actually, it’s not the academic evidence that convinces them, it’s the living, breathing evidence – hearing from the patient themselves – that changes their mind towards the efficacy of medical cannabis.”
Dr Barron continued: “There has been a growing groundswell of doctors in the UK willing to learn more about this medicine and support their patients’ interests. Cannabis based medicines such as Cannabidiol is a rapidly emerging field of medicine which is only just gaining popularity.
“It is our duty to be informed and approachable on the subject but further to that doctors now have the opportunity to develop professional skills in an area of personalised medicine which is growing rapidly.
“We encourage UK GPs to join us at PCCN and to expand our knowledge as we are just at the cusp of a huge growth area in healthcare.”
Find out more about the PCCN and read the full report here


 News6 months ago
News6 months ago
 Science5 months ago
Science5 months ago
 Industry6 months ago
Industry6 months ago
 News6 months ago
News6 months ago
 News5 months ago
News5 months ago
 Health4 months ago
Health4 months ago
 News5 months ago
News5 months ago
 Health3 months ago
Health3 months ago


















