Abby Hughes has been self-medicating with cannabis since her teens, but after a recent diagnosis of ADHD and finding out she is autistic at the age of 32, her life is only just starting to make sense.
“At school all my teachers would say, ‘Abby does fantastic work, but she needs to stop being such a perfectionist’ – I always zone in on the little details, everything has to be uniform and colour-coded.
“I collect stones with holes in them and I spent my 21st birthday looking at train stations in Stockholm,” recalls Abby.
“I’ve always been a bit of a different cog in this weird little world and nobody realised.”
These little character traits are starting to make sense to Abby now, after she was diagnosed with ADHD this year aged 32 – and just a few weeks later found out she is autistic.
As a teenager she was diagnosed with depression and anxiety, prescribed medication and therapy to manage her symptoms, but now she is starting to look at her life through a different lens.
“I was told I had anxiety and depression and found myself thrown into CBT therapies and taking various medications, but now I know it was actually undiagnosed ADHD,” she continues.
 “I wasn’t a hyperactive little boy, so nobody saw it. We need to change perspectives on what these invisible conditions are and how they actually affect you.”
“I wasn’t a hyperactive little boy, so nobody saw it. We need to change perspectives on what these invisible conditions are and how they actually affect you.”
Attention deficit hyperactive disorder affects millions of children worldwide, but boys are more than twice as likely as girls to receive a diagnosis.
According to the Child Mind Institute, women tend to be older than men when diagnosed, partly because symptoms often present differently in them than in men and are less prevalent.
Co-existing conditions, such as depression and anxiety can also cause complications which lead to a diagnosis being delayed.
Abby believes it is cannabis that has “helped her cope” for long, and may be the reason her symptoms were able to go under the radar.
“I’ve been using cannabis almost every day since the age of 14,” she says.
“It’s only now that I’m realising the extent that it has helped me to get on in the world. It has genuinely helped me cope at work and in social situations – some days I’m the life and soul of the party and others I’m just not in the mood for talking to anyone.”
She adds: “I’ve always relied on it, but I didn’t realise that it was my medication until a bit later. I’ve actually been masking for years and years using cannabis. I’m seeing it through this whole new lens.”
Growing up in Abby’s family, cannabis was known as “Nanny Carol’s herbal tea”.
“My nan always used cannabis, we knew it wasn’t allowed, like alcohol or tobacco, but we had no idea it was an illicit drug – it was just my nan’s special ‘tea’. It was never in our faces, but it was never hidden from us either.
“I started using cannabis as a teenager after I was diagnosed with anxiety and depression and realised it was helping, but I didn’t have a routine or medicate properly, I just used it in social situations.”
But as she grew up and her health became more complex, cannabis began to provide physical relief too.
When Abby went to the doctors about the debilitating pain she experienced around her period – which could last for up to 10 weeks – she was told it was just “period pain” and given the implant to prevent them at just age 15.
“I didn’t want to tell my mum in case she thought it was for contraception,” she remembers.
When she was eventually diagnosed with endometriosis in 2012, she had the coil inserted, which she describes as the “worst thing that ever happened to her”.
“I had to have it out in a matter of weeks. Now I know I’ve got a tilted pelvis and I’m hyper-mobile, no one should have been rummaging around in there, but no one picked up on it for years.”
Doctors offered her drugs such as amitriptyline, gabapentinoids and fentanyl patches, but they failed to keep the pain under control and she continued to consume cannabis illicitly – even travelling to Amsterdam to find a strain which was supposed to be good for endometriosis.
By the time Abby was referred to a rheumatologist, more than a handful of people had told her symptoms sounded like Ehlers Danlos syndromes (EDS).
She was diagnosed with fibromyalgia and hypermobility first, and then EDS at a specialist centre in London in 2017.
EDS are a group of conditions which affect the connective tissue which provides support in skin, tendons, ligaments, blood vessels, internal organs and bones.
It can affect people in different ways and in all parts of the body – for some, the condition is relatively mild, while for others their symptoms can be disabling.
Abby saw a gastroenterologist who found problems with her intestines, and a cardiology specialist who told her she had Postural tachycardia syndrome (PoTS) – which explained why she had been passing out for years and not knowing why.
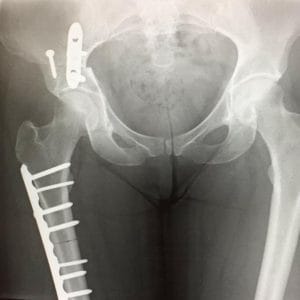
Abby underwent major surgery in 2019.
“They basically saved me because they helped me understand what the hell was going on with my body,” she says..
“There were so many different things, but one thing all of my symptoms had in common was that they were helped by cannabis.”
At the time, Abby was working as an operations manager in the NHS in complex departments such as bariatric surgery, inherited metabolic diseases, neurology and at one point managing one of Europe’s largest bone cancer departments.
After dropping out of her creative media degree after one year, she says she got her job by “pure chance” aged 21 and went from a band three straight to management as she was good at “making im
provements in managing waiting lists.”
“They took a chance on me, but I don’t know how I did it,” she says.
“At one point it was me and seven people running the largest bone cancer centre in Europe, reporting directly to the chief executive.
“I masked my way through the whole thing and ironically, I was off my face on drugs, opiates, the whole time.”
Abby ended up having a breakdown and was made redundant from her role, while on the waiting list for major orthopaedic surgery, herself.
“I lost my whole career because I got sick and they couldn’t understand why,” she says.
In February 2019, she underwent the invasive procedure, which involved cutting into her hip socket in three places as well as her femur and having metal work implanted in her legs.
Doctors warned her it would take her 10 times longer to recover due to her PoTS.
“By day three other people would be up and walking, so I was getting really frustrated,” she says.
“I told the nurses and started taking a THC oil that my friend had made. The next day I didn’t only walk, but I walked up three stairs. The nurses let me keep using the oil because they could see how it was helping me.”
Losing her job meant she was finally able to be honest about her cannabis consumption.
“I’d been doing a bit of advocacy around cannabis and I’d been carefully telling people in the NHS, asking them about the endocannabinoid system as though I didn’t know anything about it. I was finally able to come out and be a patient and be truthful about it. The law had changed but I still couldn’t afford to get a prescription.”
As of 2020, Abby now has a medical cannabis prescription, which she describes as a “life-changer”.
The same year, she helped launch PLEA (Patient-Led Engagement for Access) with a group of other patient advocates to challenge the inequalities in accessing cannabis medicines on the NHS.
“Now I’m prescribed it, I’m in an even better place. I was on Tramadol, amitriptyline, dihydrocodeine, diazepam – dozens of different drugs. They have all been replaced with CBD oil, and two types of THC flower, and that is all I take.”
“It’s been a game-changer, I can get up in the mornings and be productive.”
A few weeks ago, she shared a video of her and friend and PLEA co-founder Lucy Stafford rollerblading three miles along the coast in Brighton.
“Having a continuous source of medication is what has enabled me to go out and rollerblade as part of my recovery, something I never would have imagined was possible.”
PLEA has celebrated a number of significant achievements since its launch exactly one year ago, including hosting the first ever Medical Cannabis Awareness Week in November 2020.
The hub of the organisation, PLEA’s Patient Working Group gives patients a voice and ensures their experiences are at the centre of the UK sector as it develops.
“PLEA is completely independent and volunteer run, it is built by patients for patients, because we should be centred and amplified in this sector,” says Abby.
“There isn’t a day off for us, every day we get patients messaging us, academics wanting to speak to us, journalists getting in touch, which we are really grateful for, but it’s non-stop.
As chair and outreach director – alongside the many other hats she wears – including as a Project Twenty21 patient access consultant and a co-founder of Plant Ed Collective – it’s often taken for granted that Abby is a patient herself.
“People just see me rollerblade and think I’m fine, but I’m not. I can go rollerblading sometimes, but sometimes I need a stick to help me walk.
“I’m a patient too and it’s cannabis that has enabled me to do all this,” adds Abby.
“And I think having ADHD helps.”
In our Patient Voices series, we’re sharing the stories of members of PLEA’s Patient Working Group.
Read what medical cannabis means to Eppie, Gillian, Margaret and Jonathan
Find out more about the PLEA patient working group here & visit pleacommunity.org.uk for further resources
[activecampaign form=33]

 News6 months ago
News6 months ago
 Science5 months ago
Science5 months ago
 Industry6 months ago
Industry6 months ago
 News6 months ago
News6 months ago
 News5 months ago
News5 months ago
 Health5 months ago
Health5 months ago
 News5 months ago
News5 months ago
 Health3 months ago
Health3 months ago














