Estimated reading time: 6 minutes
Home » Health » Epilepsy » Why NHS trials won’t help the children relying on medical cannabis now
Medical cannabis campaigners have welcomed trials promised by the government this week, but they won’t help the dozens of children who need NHS access now.
Families have welcomed further promises from the government this week of two “pioneering” randomised control trials (RCTs) into the use of cannabis medicines for epilepsy.
Speaking in Parliament on Tuesday 1 March, Minister for Care and Mental Health Gillian Keegan, said the NHS and the National Institute for Health Research (NIHR) were “working closely” on two RCTs to compare the effects of medicines containing CBD, and CBD with THC, and a placebo.
“This is a pioneering area of research and I’m aware that NHS England and NIHR are working closely to get the trial started as soon as possible,” said Keegan, in response to a question brought by Christine Jardine, the Lib Dem MP for Edinburgh West.
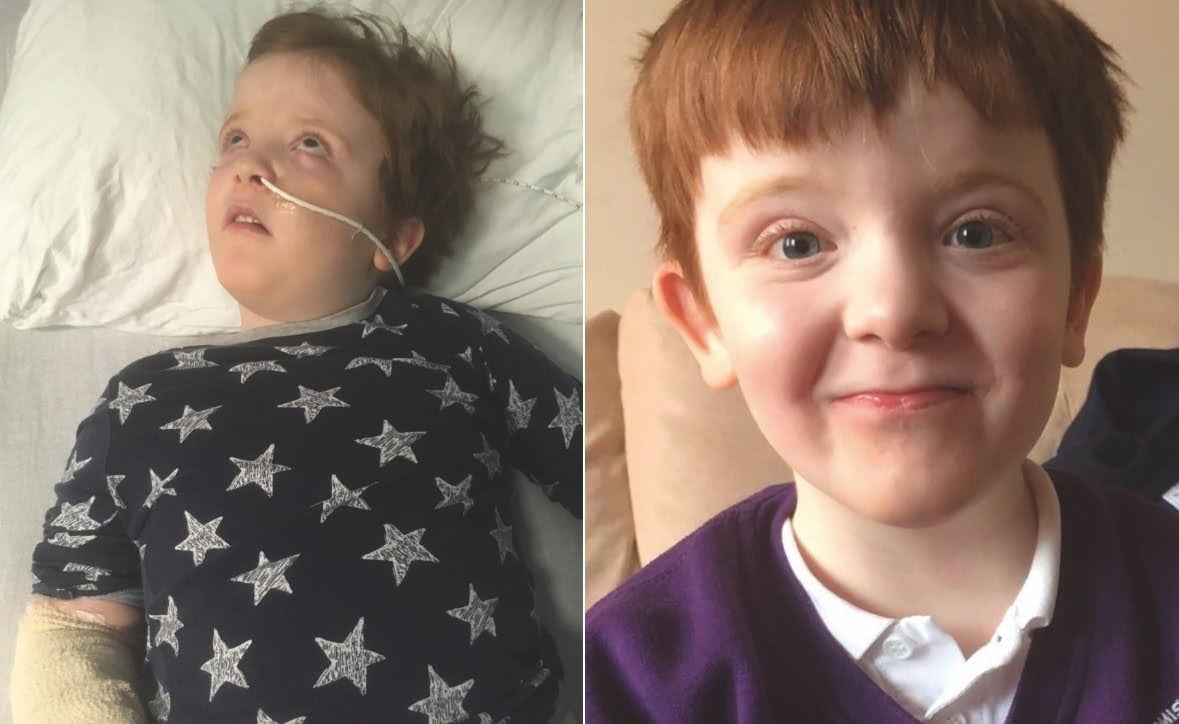
Jardine has been pushing for NHS access to medical cannabis on behalf of her constituent, nine-year-old Murray Gray, who has been seizure-free since he was prescribed the medication privately.
Murray is one of dozens of children who have been denied a prescription on the NHS, leaving their families forced to fundraise to find the hundreds of pounds needed each month to cover the costs.
“Unethical” trials
Karen Gray, Murray’s mum said the promise of NHS trials was “long overdue” but these trials will not be suitable for children like her son, who are already responding well to whole plant cannabis.
The medicines used in the NHS trials are expected to be isolated CBD and THC products, meaning patients won’t benefit from the other minor cannabinoids and terpenes found in whole plant cannabis, which make up the entourage effect.
To partake in the trials, children would also have to come off the medicines they are currently on and may end up being given a placebo.
Karen fears that Murray’s seizures would return if he stopped taking medical cannabis, which could be life-threatening for him. His condition, Doose syndrome, previously left him suffering hundreds of episodes a day.
“NHS trials are welcomed, and are three years overdue,” said Gray.
“They will hopefully be beneficial for some children who have not tried cannabis medicine, but our children rely on the whole plant oils they have been receiving for the past three years.
“They unfortunately cannot enter into these new trials as they would have to be stripped off their current cannabis oils to perhaps take a placebo. It’s unethical and I would not risk my child’s life like this.”
She added: “We need the NHS doctors to write our prescriptions, they will be writing children prescriptions for THC during the trial, therefore they should now do the right thing and write our children’s prescriptions also.”
Jardine also recognised that while these trials may help break the current “log jam” when it comes to medical cannabis on the NHS, there is still a way to go before patients like Murray have access to the prescriptions they need.
“We still have a long way to go before we have the sort of NHS support and prescriptions which children like Murray so desperately need and deserve,” she told Cannabis Health.
“For me the significance of the trials is not in its immediate impact but in moving us forward and breaking the log jam which had existed since November 2018.
“We still need to be pushing at every opportunity for NHS prescriptions to be provided for children like Murray whose lives have been transformed.
“We also need to recognise the work that is being done by British companies to establish a viable industry in this country producing medicinal cannabis oil and the difference that could make for so many people whose lives could be transformed by access to it.”
More questions than answers
Others have raised concerns that these RCTs may result in more questions than answers.
Matt Hughes, co-founder of Medcan Support, which supports families of children with epilepsy, believes the trials are not due to start until 2023 – five years since the law changed to legalise cannabis – and he believes the studies are too “narrow” in scope.
“There are some question marks over the design of these trials, it seems quite short-sighted and could potentially lead to further delays to access,” said Hughes.
“Fundamentally the NHS wants to know if THC is any more efficacious in seizure control than CBD. If an isolated THC product is no more beneficial than a CBD isolate, is that going to lead to further delays in accessing it? Is it going to lead to the NHS saying that cannabis shouldn’t be prescribed, when actually they haven’t looked at the full entourage effect?”
He continued: “Even if it is shown that THC is more efficacious, I don’t believe that will lead to the prescribing of the current unlicensed medicines. What we’ll end up with is isolated products available on the NHS, not the whole plant cannabis that is prescribed privately.”
Real-world data
Another issue is the amount of CBD and THC in the products, which Hughes believes will be a 20:1 ratio of CBD to THC.
A recent observational study carried out by Drug Science, analysed the effects of whole plant cannabis extracts in 20 children with refractory epilepsy, and was found to reduce seizure frequency by 86 per cent.
However, the average ratio of CBD to THC was 25:1 to 30:1 – and importantly, researchers think the other minor cannabinoids and terpenes were also having an effect. Tests are currently being carried out on the oils used to quantify the ratios of other cannabinoids that the children were taking.
Hughes wants to see this real-world data being used, to not only help shape clinical trials, but as the evidence itself.
“The trial design isn’t looking at what happens in the real world,” he continued.
“Real world evidence really needs to be taken into consideration here. RCTs are good, but they are a very long and expensive journey, meanwhile patients are left waiting and suffering.
“We could be prescribing cannabis [on the NHS] now, based on the current research and looking at the individual children that have benefited from it.”
Cannabis Health contacted The NIHR but they were not in a position to comment or provide further details.
NHS England and the Department of Health and Social Care had not responded to requests at the time of publication.

 News6 months ago
News6 months ago
 Science5 months ago
Science5 months ago
 Industry6 months ago
Industry6 months ago
 News6 months ago
News6 months ago
 News5 months ago
News5 months ago
 Health4 months ago
Health4 months ago
 News5 months ago
News5 months ago
 Health3 months ago
Health3 months ago