Could a deficiency of the endocannabinoid system be the root cause of ‘hard-to-treat’ conditions such as fibromyalgia, irritable bowel syndrome (IBS) and migraine? Some experts think so.
In medicine, some conditions are branded as ‘treatment resistant’ – in other words, they are health issues that for decades doctors have struggled to get to the bottom of. Conditions such as fibromyalgia, migraines and IBS are among the syndromes classed as ‘hard-to-treat’.
In a desperate attempt to find a solution that relieves their symptoms, many patients living with these diagnoses have self-prescribed cannabis, often risking legal repercussions to get access to – what to them, has always been a medicine.
It is only in more recent years that scientists have been turning their attention to the medicinal properties of cannabis, as well as the body’s puzzling endocannabinoid system (ECS).
Over the past two decades, the ECS has slowly emerged from relative obscurity to become a more widely known and increasingly researched area of medicine.

What is ECS deficiency?
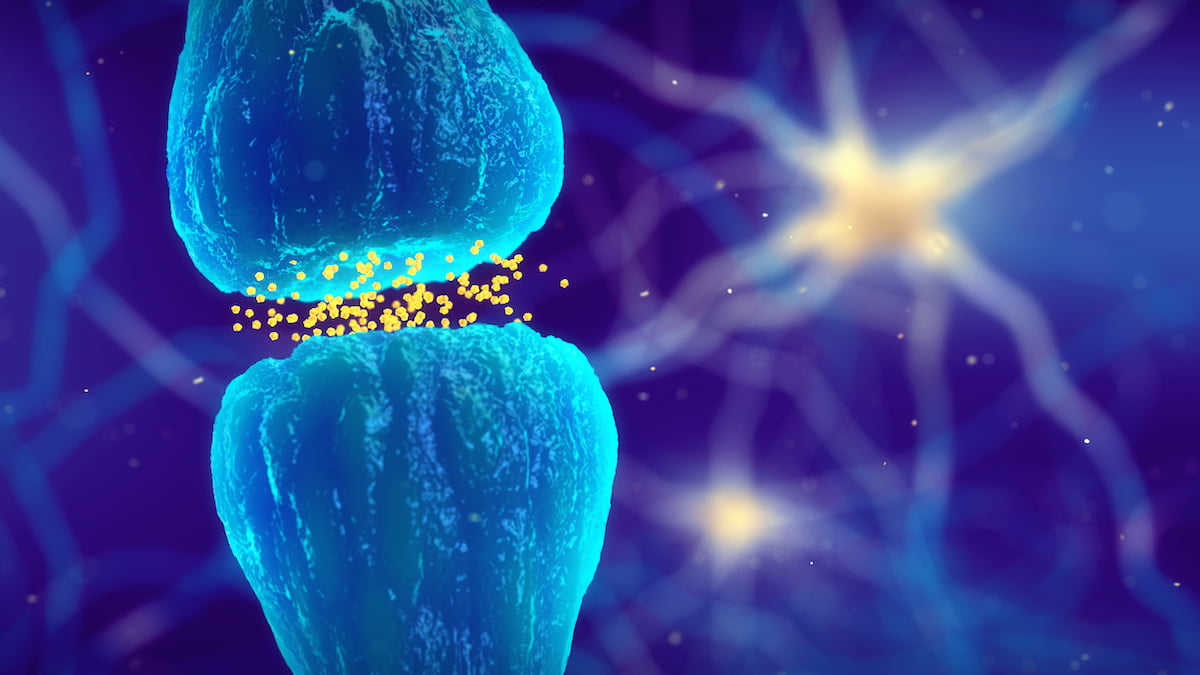
The ECS was initially discovered in the early 1990s by Israeli scientist Raphael Mechoulam, during his research into the effects of the cannabis plant on the brain and body.
What he found was a system built into all animals with nervous and immune systems, which appeared to regulate a host of different functions in the body and brain, from pain and inflammation to body temperature and mood.
Over two decades, leading cannabis expert, Dr Ethan Russo, has built on Mechoulam’s original work. In 2016, he put forward the theory of endocannabinoid deficiency as a cause of certain health conditions, particularly treatment resistant syndromes like fibromyalgia, IBS and migraine.
Dr Russo hypothesised that in some conditions, there are deficiencies in the ECS that causes the system to be under-active, or to not produce enough of the endocannabinoids needed to regulate certain functions in the body and/or brain.
He found that if a patient supplemented their ECS with molecules that emulated the chemicals that transmit information from one nerve or one cell to another – known as phytocannabinoids – then this can help rebalance the ECS and as a result improve their symptoms.
Dr Anthony Ordman, one of the UK’s senior consultants in pain medicine, and an experienced prescriber of medical cannabis, believes the theory carries some significant weight.
“I find it a very helpful hypothesis, both for helping doctors to understand how to use cannabis medicine, but also to help patients to understand what we’re trying to do,” Dr Ordman told Cannabis Health.
“In other words, they’re not necessarily medicines like morphine that actually do something, rather their purpose is in helping the body rebalance.”
He continued: “Cannabis can reduce long-term stress, which is often present in fibromyalgia patients and it can relax muscle tension and normalise sleep, which is always badly affected in [the condition].
“This concept of rebalancing the body explains how one simple group of chemicals can have so many beneficial effects. It’s not because it’s magic or mystical – it’s because it helps bring the body back to normality.”
Is this why CBD works so well?
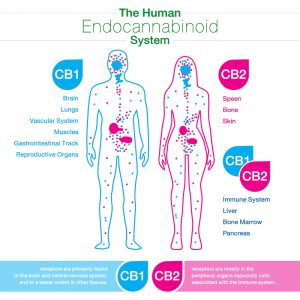
The key elements of the ECS that affect people’s health are the endocannabinoids, anandamide and 2-arachidonoylglycerol (2-AG), as well as the relative abundance and state of cannabinoid receptors, CB1 and CB2.
Dr Elisabeth Philipps, a neuroscientist specialising in the ECS, said of the theory: “It is still quite controversial in some ways, because the ECS is not widely understood, but in terms of fibromyalgia, IBS, migraine, what they call the treatment-resistant syndromes, I think an endocannabinoid deficiency is contributing.
“I think that’s why CBD works so well for so many people in so many different conditions. It’s not by chance that somebody might take CBD for pain and somebody might take CBD for sleep. It’s because there are widespread deficiencies.”
She added: “There’s some really good work around how migraine is probably partly to do with endocannabinoid deficiency and our body not producing enough 2-AG or anandamide which the body needs for the ECS to function.”
One of the many areas of ECS research that remains incomplete, is where deficiencies in the system come from and whether certain conditions are caused by specific chemical imbalances.

Dr Elisabeth Philipps
Some theories suggest genetic makeup plays a role in people’s susceptibility to certain conditions, while others look to lifestyle choices as a possible cause.
What is clear, is that the ECS is likely to become central in scientists’ further understanding of these conditions.
“We know that multiple systems are going to be affected in conditions like fibromyalgia, which is why in conventional medicine, it’s so difficult to treat,” Dr Philipps explained.
“What we don’t know at the moment is specifically why there’s a deficiency in any of the systems – the ECS included.
“But what we do know is that by using cannabinoids, it is going to support areas like anxiety, sleep, and pain. For conditions like fibromyalgia, supporting the ECS function is going to be very much part of the picture of providing wellness.”
A holistic approach
Although compounds found in cannabis have been shown to help regulate people’s ECS, Dr Philipps stressed that medical cannabis is just part of the picture.
“We need to be looking at these conditions more holistically,” she said.
“For example, chronic stress down-regulates the ECS. We can see that there are lower levels of endocannabinoids in people who are chronically stressed.
“We can put more cannabinoids into the body, but at the end of the day removing that stress is going to help balance the body more naturally.”
For Dr Philipps, cannabis products should be part of a holistic approach to the ECS, that gets to the “root cause” of the issue.
By continuing to research the system, scientists should hopefully be able to further understand hard-to-treat conditions and how they can be improved, she said.
“Often, you take a painkiller and it’s a bit like a plaster; you don’t really get into the root cause,” she explained.
“Using CBD or medical cannabis you are getting to the root, because you are treating or supporting the body’s ECS to work more effectively.”
Dr Philipps added: “These conditions are so widespread, from migraine to IBS, hundreds of millions of people who suffer every day don’t necessarily get the answers that they need from a conventional medical approach.
“If we know more about deficiencies and ECS, we can understand more about how we can support it through medications or supplements.”
Home » Health » ECS deficiency – the root cause of ‘hard-to-treat’ conditions?

 News6 months ago
News6 months ago
 News6 months ago
News6 months ago
 Science5 months ago
Science5 months ago
 Industry6 months ago
Industry6 months ago
 News6 months ago
News6 months ago
 News5 months ago
News5 months ago
 Health4 months ago
Health4 months ago
 News5 months ago
News5 months ago